Research Article
Intravenous Thrombolysis in Acute Ischemic Stroke: A Combined Audit and Young Stroke Subgroup Analysis from a Tertiary Centre in Northeast India
Bhutada A
Department of Neurology, GMCH Guwahati, Assam, India
*Corresponding author:Dr Akshay Bhutada, Department of Neurology, GMCH Guwahati, Assam, India Email Id: akshaythegiant@gmail.com
Article Information:Submission: 07/06/2025; Accepted: 22/07/2025; Published: 24/07/2025
Copyright: ©2025 Bhutada A. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Background:Intravenous thrombolysis (IVT) is a well-established treatment modality in acute ischemic stroke (AIS), yet its realworld implementation varies regionally, especially in resource-limited settings like Northeast India. Furthermore, stroke in young adults (<50 years) represents a distinct subgroup with different etiological and outcome profiles. Intravenous Alteplase 0.9mg/kg was given in eligible patients.
Objective:To conduct a comprehensive audit of thrombolysis practices at a tertiary care center and to analyze clinical outcomes among young stroke patients undergoing IVT.
Methods:This retrospective observational study was conducted at the Department of Neurology, GMCH Guwahati. Among 444 ischemic stroke admissions, 29 patients received IVT between 2023 and 2024. Of these, 7 patients were under 50 years. Demographic, clinical, radiological, and outcome parameters were analyzed.
Results:The median NIHSS score before thrombolysis was 15. MCA territory involvement was universal. Post-thrombolysis NIHSS improved in 82.7% of cases. Overall mortality was 17.2%. Among young patients, the most common etiology was small vessel disease (TOAST Class 3), with favorable outcomes (mRS ≤2) in 57.1% and mortality in 28.6%.
Conclusion:IVT in AIS offers tangible functional benefits, including in younger adults. High mortality among young stroke despite early treatment emphasizes the need for early diagnosis and comprehensive care pathways.
Methods:This retrospective observational study was conducted at the Department of Neurology, GMCH Guwahati. Among 444 ischemic stroke admissions, 29 patients received IVT between 2023 and 2024. Of these, 7 patients were under 50 years. Demographic, clinical, radiological, and outcome parameters were analyzed.
Results:The median NIHSS score before thrombolysis was 15. MCA territory involvement was universal. Post-thrombolysis NIHSS improved in 82.7% of cases. Overall mortality was 17.2%. Among young patients, the most common etiology was small vessel disease (TOAST Class 3), with favorable outcomes (mRS ≤2) in 57.1% and mortality in 28.6%.
Conclusion:IVT in AIS offers tangible functional benefits, including in younger adults. High mortality among young stroke despite early treatment emphasizes the need for early diagnosis and comprehensive care pathways.
Keywords:Ischemic Stroke; Thrombolysis; Young Stroke; TOAST; NIHSS; mRS; MCA Infarct
Introduction
Stroke remains one of the leading causes of mortality and longterm
disability worldwide, particularly in low- and middle-income
countries (LMICs) like India. Acute ischemic stroke (AIS) constitutes
the majority of all stroke cases, and intravenous thrombolysis (IVT)
with recombinant tissue plasminogen activator (rtPA) has been
shown to significantly improve outcomes when administered within
the therapeutic window.
Despite well-established national and international guidelines,
thrombolysis is underutilized in India due to delays in hospital arrival,
lack of awareness, diagnostic limitations, and resource constraints.
Regional audits are essential to understand local challenges and
outcomes. Furthermore, young stroke—a distinct clinical subset
defined as stroke occurring before the age of 50—presents unique
etiologies such as vasculitis, arterial dissection, and thrombophilias,
and demands tailored strategies.
This study combines a clinical audit of all thrombolysed AIS
patients at our tertiary care stroke center with a detailed subgroup
analysis of young stroke patients. Our objective was to evaluate
the demographic, clinical, and radiological features, etiological
subtypes, and early functional outcomes, particularly focusing on the
implications of IVT in young adults.
Materials and Methods
Study Design and Setting: This was a retrospective observational
study conducted at the Department of Neurology, Gauhati Medical
College and Hospital (GMCH), Guwahati, Assam. The study analyzed
patients treated between January 2023 and December 2024.
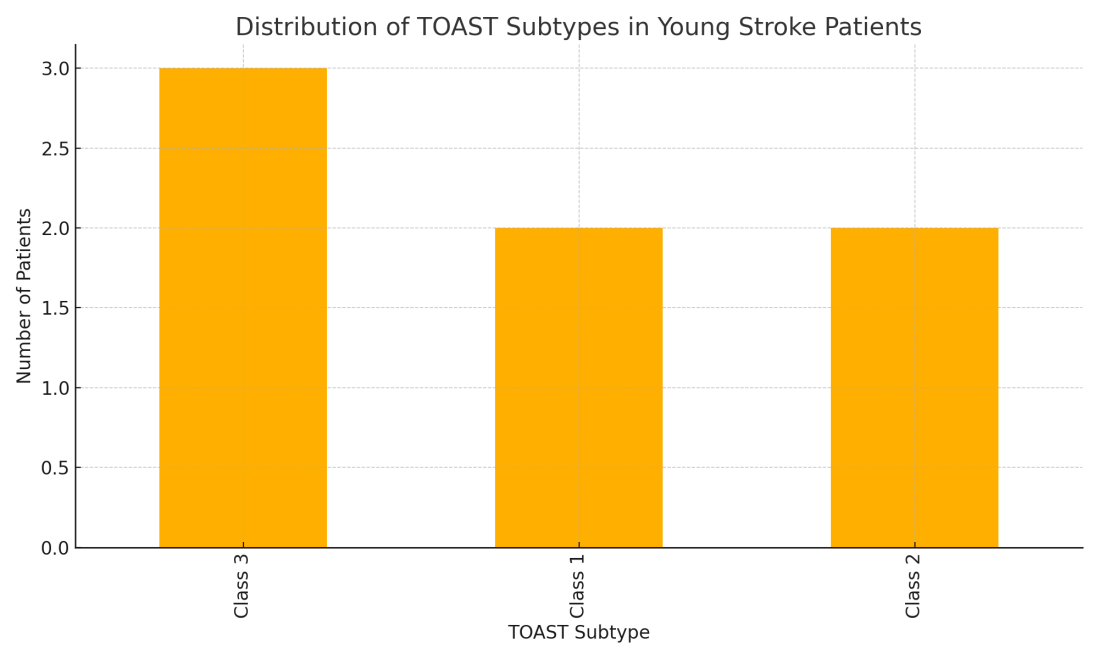
Figure 1:Distribution of TOAST Subtypes in Young Stroke Patients.
This figure demonstrates the predominance of small vessel disease (Class
3) among thrombolysed young stroke patients in our cohort.
Study Population:
Out of 444 patients admitted with acute ischemic stroke (AIS),
29 patients received intravenous thrombolysis. Of these, 7 were
under the age of 50 and were analyzed separately as the young stroke
subgroup.Data Collection:
Clinical records were reviewed to collect demographic variables,
vascular risk factors (hypertension, diabetes, valvular heart disease),
infarct territory, TOAST classification, pre- and post-thrombolysis
National Institutes of Health Stroke Scale (NIHSS), modified Rankin
Scale (mRS) scores at discharge, and in-hospital mortality.Definitions:
- Young stroke: Age less than 50 years.
- Favorable outcome: Defined as mRS ≤2 at discharge.
- TOAST classification: Used for etiological subtyping (large
artery atherosclerosis, cardioembolism, small vessel occlusion, other
determined cause, and undetermined cause).Statistical Analysis:
Descriptive statistics were used to summarize data. Categorical
variables were presented as frequencies and percentages; continuous
variables as means or medians with ranges. No inferential statistics
were applied due to the small sample size.Results
Among the 444 ischemic stroke patients admitted during the
study period, 29 received intravenous thrombolysis. Of these, 62%
were male. The median NIHSS score at admission was 15 (range
5–32). Middle cerebral artery (MCA) territory involvement was
universal (100%), followed by posterior cerebral artery (PCA) in
38% and anterior cerebral artery (ACA) in 10%. Post-thrombolysis
improvement in NIHSS was observed in 82.7% of patients. Overall,
62% achieved favorable outcomes (mRS ≤2), while 17.2% (n=5) died
during hospital stay—primarily due to hemorrhagic transformation
or sepsis.
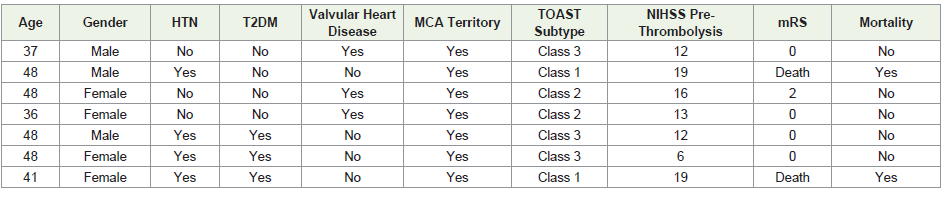
In the young stroke subgroup (n=7), mean age was 43.7 years
with a slight female preponderance (M: F = 3:4). The most common
etiological subtype was small vessel disease (TOAST Class 3), and
MCA involvement was seen in all cases. Favorable outcome was
achieved in 57.1% (n=4) and mortality in 28.6% (n=2). Valvular heart
disease was present in 3 patients.
Discussion
Our study highlights the clinical profile, etiological subtypes, and
outcomes of thrombolysed AIS patients in a tertiary care center in
Northeast India. A key observation was the predominance of MCA
infarctions across the cohort. Favorable functional outcomes (mRS
≤2) were achieved in 62% of patients, consistent with prior Indian
and global studies demonstrating the effectiveness of timely IVT
[1-4]. The mortality rate of 17.2% in our cohort is within expected
ranges, although room for improvement persists.
The young stroke subgroup represents a unique population.
While stroke in younger individuals is less common, it has
distinct etiological contributors including small vessel disease,
cardioembolism, and vasculitis. In our cohort, small vessel disease
was the leading etiology (TOAST Class 3). Notably, despite younger
age and fewer comorbidities, mortality in this group was 28.6%,
underlining the need for targeted preventive strategies and earlier
identification.
Valvular heart disease in three of seven young stroke cases
reinforces the need for echocardiographic screening in selected
patients. Previous Indian series have similarly emphasized
cardioembolic contributions in young stroke [5,6]. The functional
outcome profile among young stroke patients in our audit was
moderately favorable, aligning with existing literature [7,8].
Another important observation is the high proportion of patients
presenting within the thrombolysis window—highlighting improving
awareness and pre-hospital care. However, logistical barriers like
delayed imaging and financial constraints still hinder broader
implementation, consistent with other Indian data [9,10].
Conclusion
Intravenous thrombolysis significantly improves early
neurological outcomes in AIS patients. In this single-center
experience from Northeast India, MCA strokes predominated and
outcomes were generally favorable with early intervention. Stroke
in young adults, although comprising a small subset, poses unique
challenges and outcomes. Regional audits like ours are vital to inform
health policy, optimize acute stroke care delivery, and drive public
awareness.
Declarations:
Funding: Not applicable.Ethics Approval and Consent to Participate: This was a retrospective audit of anonymized data; formal approval was waived. Consent for Publication: Not applicable.
Competing Interests: The authors declare that they have no competing interests.
Availability of Data and Materials: Available from the corresponding author upon reasonable request.
Author Contributions: Dr. Akshay Bhutada: Conceptualization, data curation, formal analysis, and manuscript preparation.
References
Citation
Bhutada A. Intravenous Thrombolysis in Acute Ischemic Stroke: A Combined Audit and Young Stroke Subgroup Analysis from a Tertiary Centre in Northeast India. Indian J Neurol. 2025;6(1): 147.